Emergency Movement Medicine for Low Back Pain
Lab #3 took place at Imperium CrossFit in Houston, Texas after the Just Roll With It Boot Camp Seminar. Dr. Larson worked with a Veteran and adaptive athlete named Tim Brumley (see video) who had recently hurt his lower back after performing the Memorial Day Warrior WODs and some heavy dead-lifting.
This Lab will focus on Acute Low Back Pain and what to do about it!!
So…have you ever bent over to pick up your kid, dead lift, front squat, or snatch with poor form and or too much weight? Have you ever tried to pull a massive object like a boulder out of your driveway (hmm… my dad), carry a guy on your shoulders who is 2 X your weight (hmm…ME), and or pick up your baby after having a C-section and feel your back give out? Perhaps all you wanted to do was curl up in a ball and cry? 
Do you have an athletic trainer who stalks you or is like your body guard? No? Really…why not! Just kidding, neither do I!
You are not alone! Millions of individuals in the United States suffer from acute low back pain for various reasons every year. Roughly $100 billion is spent every year on acute (7-14 days post injury) low back pain injuries according to the Journal of the American Osteopathic Association. [1] Chronic (3-4 weeks and up to 6 months post immediate injury) injuries are a whole different ball game and are also up there in terms of the billions of dollars spent in our health care system. These chronic conditions usually occur when the reason for the acute condition was not taken care of immediately!
These acute low back pain symptoms can range from spasms, burning pain down the leg, a centralized pain in the low back and/or butt region, or aching pain at the base of the spine. The pain may feel like a hot spot or like none of the muscles in your back are working. We all can call our primary care physician and get the top ten list of what medicine to take for the pain – naproxen, ibuprofen, even Vitamin M (military term for Motrin). But what can you do aside from ingesting pills to help alleviate the immediate symptoms that sometimes take you out of the game and literally lie you flat on your back with disbelief? Of course there are positions and lifting techniques to master, but for this short period of time, when you feel like you are in the twilight zone or the pain cave, let’s get you moving correctly!
As a sports medicine and performance-focused doctor of physical therapy, if you were my client -OR if I were still in the Marines and you were in my platoon or company – I would work to rectify the situation with proper movement, regardless of the issue. Vitamin M (Motrin) would be out of the question and we would seek to relieve the immediate symptoms with how you position yourself. Let me be clear that we are NOT taking into account any central nervous system damage, other traumas, or diseases such as ankylosing sponydyolysis, spinal osteoblastomas, osteoporosis, osteonecrosis etc. Rather we are talking about musculoskeletal injuries such as vertebral disc herniations, bulges, facet joint dysfunction, spondylolysis, sprains in the ligaments, or strains in the muscle supporting the spine. These injuries happen, and your doctor, physical therapist, chiropractor, coach, mommy or daddy may not be there or know how to coach you through what to do next, so here it goes!
Keep in mind all these techniques are to help get you back to moving correctly so you can function. It is merely a band-aid. The main thing to address is WHY this did happen in the first place. Those reasons are overuse, poor form, too much weight, or all of the above!
BACK SPASMS
If you have been having low back spasms for a few days from an overstressed muscle, sacroiliac joint dysfunction (a literal pain in the butt and your hips feel off), possible vertebral disc issue (the jelly doughnut between each spinal segment), or from a number of other symptoms, then check out the following video. Note: If your back “spasms” become debilitating or start radiating down your leg, or you feel numbness and tingling, please consult your primary health care professional to help you with a condition that might be more serious that you think.
Beyond what’s in the video, help the tissues of the back relax by applying heat in the form of a pad or a soak in a hot tub or bath. The strain-counter-strain is a good technique that can help alleviate muscles that are having spasm episodes or have a knotted feeling, but I am not demonstrating this in the video.
SPONDYLOLYSIS
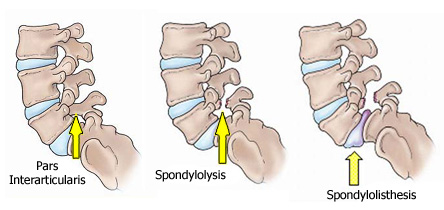 (taken from orthoinfo@aaos.org)
(taken from orthoinfo@aaos.org)
A spondylolysis is defect or fracture of the pars interarticularis on the lumbar spine (see picture above), which surprisingly does not always express symptomatically. This fracture can turn into a spondylolisthesis which is a slippage of the vertebral body forward and can implicate the spinal cord if not taken care of IMMEDIATELY! This slippage is usually where the symptoms come from and can range from a hot spot like feeling, or numbness and tingling and or an aura of instability in the low back when performing any lifts from the ground!
Spinal stability (otherwise known as core stability) is essential as well as any activity that will help improve dynamic strength. By spinal stability I mean hips, low back, and abdominal’s; they all attach to your spine in some shape or form.
Find a health care professional who can help give you the appropriate dosage of load of exercise and trunk work (core) for the condition you have. This condition can happen due to a tackle in a football game, coming off a layup, and or performing an Olympic Lift with an already excessive overextended posture. Usually this happens at the Lumbar level 5-Sacral level 1 vertebral segments.
The name of the game – SPINE-and CORE STABILITY! As stated in the Journal of American Academy of Orthopedic Surgeons, “Current evidence suggests that decreased core stability may predispose to injury and that appropriate training may reduce injury.[2]” Do not try, I repeat DO NOT try to self diagnose and treat. Spinal cord damage can occur with a condition like this, if not take seriously! Invest in an evaluation and treatment program.
SPRAINS, STRAINS, and the LUMBAR DISC
The third issue I am going to discuss is low back pain that comes on after you pull, push, or apply a load to your low back that freaks it out and makes you want to curl up in a ball. Whether I was a Marine Corps lieutenant or DPT evaluating you (I am both), I’d tell you to “GET UP AND STAND UP STRAIGHT!! “ Do not curl up in a ball, and do not go to bed crying into your pillow in a flexed position! 
Sure you may have had something like this before but remember it being less aggressive or painful, and you attempt your best self diagnosis. You may be quite certain it is your psoas major, or a lumbar strain, or you just know you were lifting with piss-poor form. No matter the self-diagnosis, stand up and keep that spinal curve in check. Do not overextend, do not flex forward, just stand up and maintain a neutral spine. As Dr. Kelly Starrett mentions in all his mobility and movement seminars and in his new book, Becoming a Supple Leopard, squeeze your butt as if your life depended on it! Whether it is a disc herniation, a fracture, a sprain or strain, give the structures in the back of your spine a chance to approximate the tissues, disc, and ligament’s versus tear further!
Like I mentioned before, this article is for acute conditions that are following an immediate low back injury at the gym, at home, doing yard work….anywhere. Take the immediate steps to not hurt yourself further and get some professional help on HOW to fully heal and fix the reason WHY this happened in the first place!
In an upcoming lab I will talk about ways to improve spinal stability that will ultimately be your shield of protection throughout the rest of your life!!
[1] Crow TW, Willis DR; JOAOA: 2009; 109, 229-233. Available from: American Osteopathic Association. Accessed June 2013
[2] Wilson JD, Dougherty CP, et al. JOAAOS: 2005, 13: 316-325. Available from: American Academy of Orthopaedic Surgeons. Accessed June 2013.
To Access .Back Pain Exercises you can do on your own, View Now.